CMS 1500 Health Insurance Paper Claim Forms (02/12) FREE Priority Shipping
$29.00 – $49.00
The CMS 1500 is the standard claim form used by health care providers to bill for services.
• Commercially Printed on 8.5″ x 11″ paper – 20 # white bond
• Laser cut sheets for use in inkjet or laser printers
• OCR “dropout” red ink for processing on scanner equipment
• Instructions for government/private health programs on back
• Accommodates National Provider Identifier (NPI) reporting
• CMS-1500 (02-12) OMB Approved – OMB 0938-1197
Shrink wrapped in packs of 200, 300 or 500 sheets.
Description
Order sets of 200, 300 or 500 commercially-printed CMS 1500 paper claim forms. The CMS 1500 (HCFA) is the standard paper claim form accepted by most insurance carriers. The correct and current version is indicated at the top of the form where it states, “Approved by National Uniform Claim Committee (NUCC) 02/12, and in the bottom right corner, “Approved OMB-0938-1197 Form 1500 (02-12). It has been revised by the National Uniform Claim Committee (NUCC) to accommodate the new ICD-10 codes.
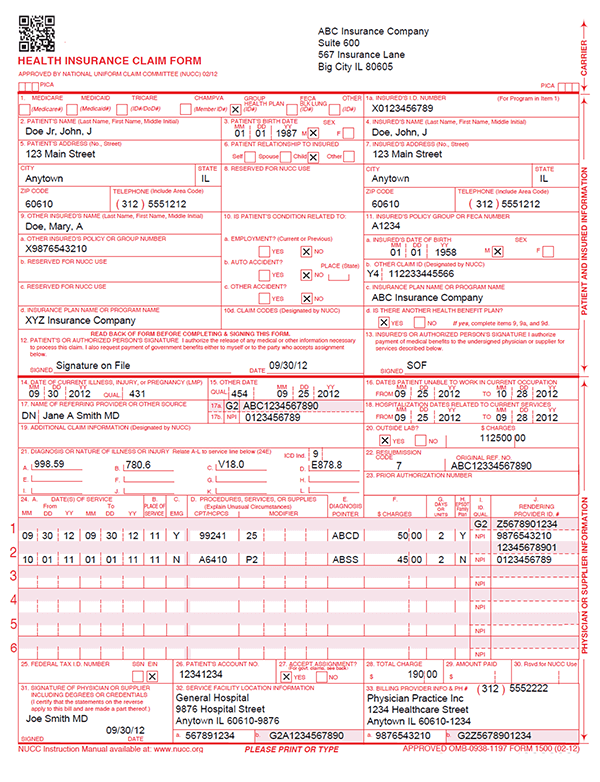 The claim form itself is split into three sections: Fields 1-13 are for patient information; fields 14-24 are for procedural and diagnostic information related to services provided; and fields 25-33 are for servicing and billing provider information.
The claim form itself is split into three sections: Fields 1-13 are for patient information; fields 14-24 are for procedural and diagnostic information related to services provided; and fields 25-33 are for servicing and billing provider information.
Paper Claim Submission Requirements. All paper CMS-1500 claims must be submitted on standard red claim forms. Black and white versions of these forms, including photocopied versions, faxed versions and resized representations of the form that do not replicate the scale and color of the form required for accurate OCR scanning, will not be accepted and will be returned with a request to submit on the proper claim form.
The CMS 1500 paper claim is used by acupuncturists, nurses, optometrists, physicians, psychologists, therapists, home health care providers, and other health care practitioners submitting a bill for services.
Paper claim forms will be shipped within 24 hours with free USPS Priority shipping.







Reviews
There are no reviews yet.